
Relationships in health settings
by Marguerite Guiguet
1. Introduction
In order to improve health and well-being, people are encouraged to take an active role in health decisions. Health promotion includes prevention, physical activities, nutrition and any activities that contribute to a healthy life. However, for individuals suffering from chronic diseases, the need for long-term medical follow-up is challenging and a lot of healthcare is centred around the diseases and their treatment. If we assume that very few people suffering from severe illness refuse treatment, the offers of care by healthcare providers are made in the best interest of the patient, how do we explain why people who are prescribed medicines do not always complete the course of treatment or do not follow recommended healthcare activities, as is frequently reported. A lack of health literacy, defined as ‘the ability to obtain, process, and understand health information needed to make informed health decisions’, has been suggested. However, other difficulties could also be explored related to the need to take control following the occurrence of health problems when both the illness and the healthcare provider take over your life. In this article we will discuss some aspects related to the communication of health information and ‘patient–provider’ relationships with reference to a French community-based survey designed by and for women living with HIV: the EVE study.
2. The EVE study
In 2011, during the ‘Positive women in action!’ workshop organised by AIDES, the main HIV/AIDS organization in France, participants had the opportunity to talk about adverse events they experienced due to their illness and their difficulties in dealing with them day after day. Many women felt that the dosage of their medication was too high as the clinical trials that had tested the drugs and decided on the dosages had mainly included men. More generally, women reported feeling that they were not listened to by their healthcare provider and that they were coping with these issues alone. This question was recognised as crucial because it was indicated as a cause for women stopping their treatment even though anti-retroviral therapy (ART) is a cornerstone of HIV care. Guidelines based on a recent clinical trial have recommended starting ART for all people living with HIV. The goal of ART is to stop the human immunodeficiency virus (HIV) from making copies of itself in the body; this is called viral suppression. Because ART reduces the amount of the virus in the body, it decreases the risk of serious HIV-related illnesses and also decreases dramatically the risk of HIV transmission associated with sexual intercourse. But up to now, ART uses daily pills and starting treatment means making a lifelong commitment because previous trials of treatment interruption have failed. In fact, in the weeks following ART interruption, the HIV virus begins to multiply again. Therefore, HIV infection management relies on retention in medical care and long-term adherence to treatment. This requires that people living with HIV trust their physician. Conversely, perceived side effects and the low attention paid by the physician to these side effects have been reported to be detrimental to the quality of the patient–healthcare provider relationship.
This is why, after the ‘Positive women in action!’ workshop, a group of women decided to conduct a study on the adverse events experienced by women living with HIV, in partnership with researchers and practitioners. The first objective was to document the magnitude of common side effects in order to help with recognising them and to improve the discussion between women and their healthcare providers.
An anonymous online questionnaire was freely accessible through a community-based website for one year (September 2013 to September 2014). The anonymous questionnaire included the HIV Symptom Distress Module (SDM) which asks about 20 symptoms and their impact on professional, social and personal lives. A given symptom was classified as ‘bothersome’ if the woman answered, ‘During the past 12 months, I have this symptom, and it bothers me/it bothers me a lot’.
Overall, 301 women living with HIV and on ART took part in the study. Their mean age was 48 years, and their mean duration on ART was 13 years, with 46 (15%) having been on it for more than 20 years. All the respondents reported to have had at least one symptom during the previous year, and the median number of symptoms experienced was 12,* with a median of 8 bothersome symptoms. As shown in Figure 1, the most troublesome symptom was fatigue reported by 73%. Newer forms of ART are supposed to have better gastrointestinal tolerance than earlier ART but symptoms such as bothersome bloating, abdominal pain, or gas were nevertheless reported by 54% and diarrhoea by 33%. Pain, memory problems, depression, anxiety and sexual issues were also frequently reported. Nearly half of the women endured a negative impact on their lives following body shape changes such as fat deposits or weight gain.
* This means that 50% of respondents reported fewer than 12 symptoms and 50% of respondents reported 12 or more symptoms.
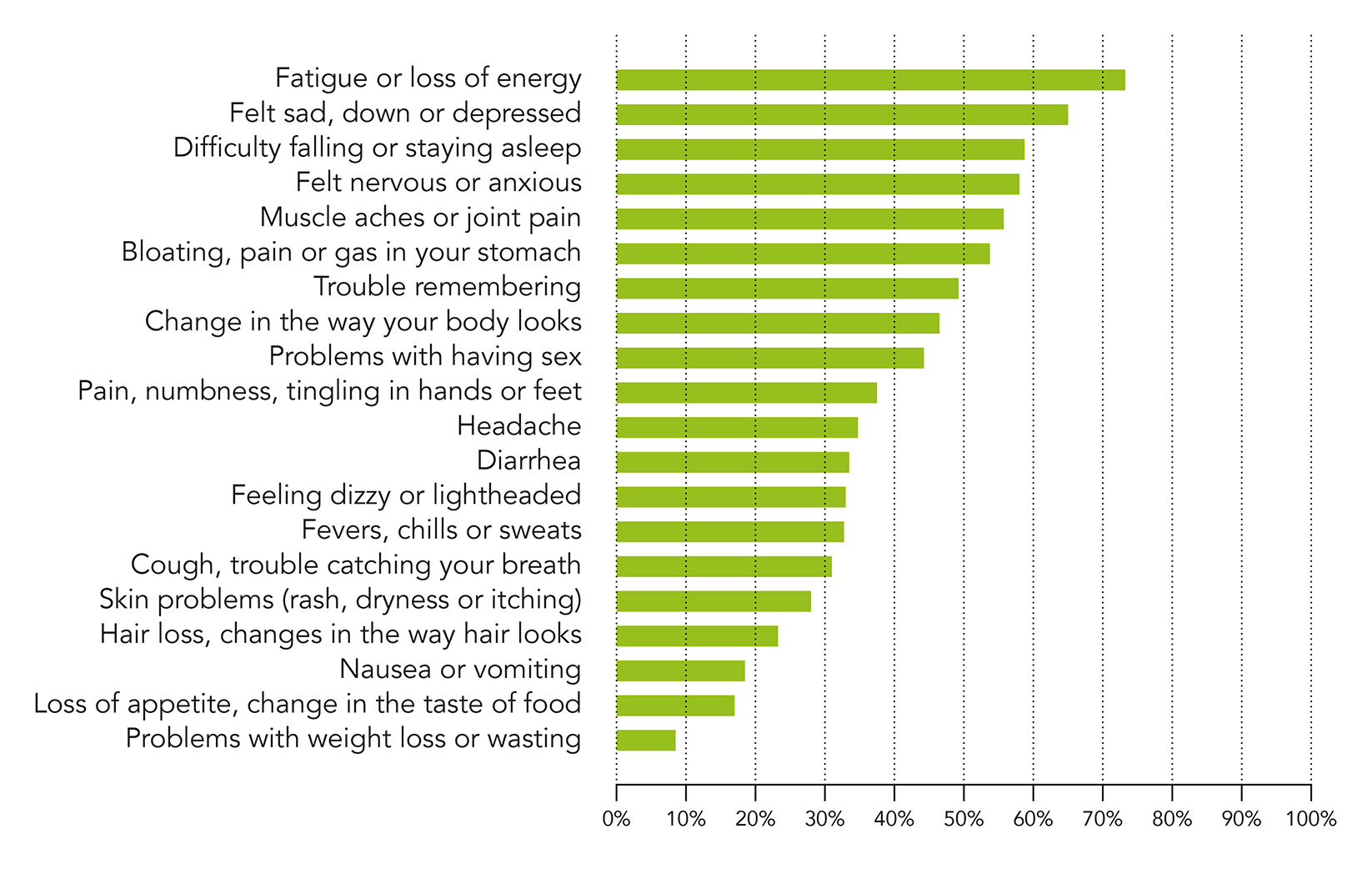
Figure 1: Proportion of women living with HIV who have experienced bothersome symptoms during the previous 12 months reported in the EVE study.
The second objective was to look at the communication between the women and their care providers on the topic of these side effects. Although 80% reported that their healthcare provider was sympathetic to these side effects, the proposed solution was mainly to contact another specialist or to take additional drugs. The difference between the support that was offered and women’s expectations is illustrated by cascades of communication from feeling to talking, and being listened to (Figure 2). Among the women who reported bothersome symptoms such as fatigue, bloating and other pain in their stomach, or changes in the way their body looks, around 80% declared that they had talked to their doctors about this issue. When it comes to sexuality, less than 30% who declared a negative impact on their lives due to problems with having sex have talked about this in the medical care setting. However, only half of the women who initiated such a discussion, whatever the side effect, felt that their doctor had really listened to them. In order to improve their tolerance, 72 (24%) women reported having made a change to their ART regimen, for example by decreasing the dosage or spacing out their drug intake, but only one out of four did so in agreement with their physician, half of them informed their physician afterwards and one in four never talked about it.
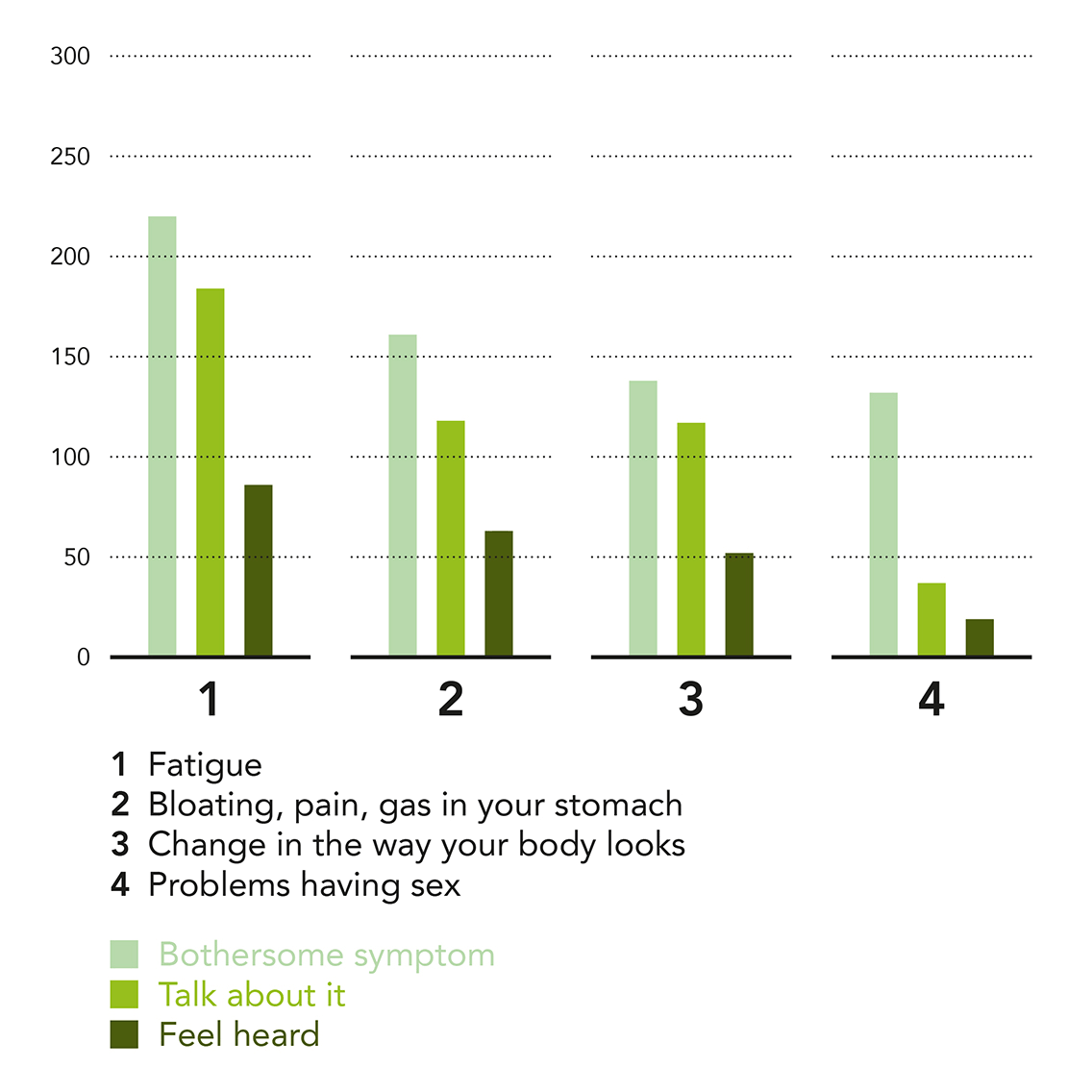
Figure 2: Cascade of communication between women living with HIV and providers around perceived side effects reported in the EVE study
This study raises issues about communication between women living with HIV and their healthcare providers concerning the side effects of their long-term treatment. In the next section we look at the communication of health information and then how education is used to shift the focus from observing the relationships to learning both by patients and medical staff.
3. Communication of health information
Communication of health information could contribute to improving relationships in healthcare settings by fighting knowledge inequalities. Efforts have been made to better understand health information with the goal of improving its usability. In the US, the Centers for Disease Control and prevention provides fact sheets and self-help documents dedicated to specific diseases and their management written in English and Spanish that have been written using the results of research in health communication and health literacy.
Some websites have been developed to present general health information while also emphasising well-being and fitness, while others are dedicated to a given condition and maintained by specific patients’ associations. The internet is now used so much as a main source of information on health that it has been proposed to use the number of queries searched online in the Google search engine, to detect outbreaks of infectious diseases such as flu.
4. Therapeutic Patient Education (TPE)
Different types of communication have been investigated one of which is downwards communication by healthcare professionals, i.e. one way communication from the professional to the patient because the non-adherence to a medical prescription has been interpreted as a lack of a patient’s knowledge. Therapeutic Patient Education (TPE) programmes have been developed, mainly for chronic conditions. The international journal, Patient Education and Counseling, is specifically dedicated to this topic and includes research on didactic methods. As presented by Perdriger and Michinov (2016) ‘TPE requires a shift from an asymmetrical physician–patient relationship to an education–oriented partnership that involves the patient and relatives in the management of the disease’. TPE programmes, also labelled as ‘self-management educational programmes’, are usually based on interactive sessions provided in small groups where patients are actively involved. An example of a new method for delivering TPE is the eLearning module on the platform ‘Bepatient’. This website uses information technologies and the use of connected devices as tools for individualised programmes of TPE provided through different supports that have been individually customised by the healthcare professional. However, evaluation of interventions based on intense education and counselling showed rather disappointing effectiveness. The Cochrane Database of Systematic Reviews has published a large synthesis of 182 interventions to improve patient adherence to treatments in different conditions. While all the studies were randomised controlled trials comparing the intervention to the standard of care, a design that is considered as the highest level of proof, no conclusive evidence of any benefit was observed. As stated by the authors ‘It is possible that interventions to date are not very effective since we do not understand in sufficient detail exactly what the adherence problems are’, highlighting the gap that exists between guidelines and the difficulties people are facing.
5. Patient–provider communication
To reduce the asymmetry in the relationship between healthcare providers and patients that could make it difficult for providers and patients to make decisions together, the health platform ‘Patient’ provides ‘Decision aids’, evidence-based advice for specific conditions and medical choices with option grids. In France, a web-site called « Deuxième avis » has recently gone online. It enables people to ask for another medical opinion before making a decision about accepting the treatment or surgery proposed for a serious illness. This second opinion is given by a specialist of the disease and based on personal data contained in the individual’s medical record. Interestingly, the possibility of asking the specialist questions is cited among the major benefits of this online consultation: questions to understand the illness, questions to understand treatment and alternatives, and ‘any questions you would like to ask’. This suggests that understandable health information may not always be provided routinely.
Patient–provider communication is also challenged when the two sides are not sharing the same story. The British Medical Journal (BMJ), a major medical journal, now has a ‘patient editor’ and has established a monthly patient-led and patient authored series, ‘what your patient is thinking’. In this series, patients set the learning outcomes for medical readers, with for example, a text written by an ‘obese patient’ explaining how she resents being viewed not as a person but as a health problem. A health education programme directed towards healthcare professionals includes a specific e-learning module for shared decision-making with the aim of shifting from an environment of medical paternalism to a more inclusive approach.
6. The role of people with experience of long-term illness
By living with long-term illness, many people develop expertise on their medical conditions. In the UK, the Long-term Medical Conditions Alliance (Wilson, 1999) has advocated for building true partnership between patients and healthcare professionals, leading to the development of expert-patient programmes based on courses tutored by trained lay leaders, rather than health professionals. A charity ‘Self-management UK’ working with the NHS delivers trained peer tutors to lead self-management interventions for chronic diseases and has also developed online programmes. Interestingly lay-led programmes would include teaching techniques to improve communication with clinicians.
Some websites expand health information communication between people sharing a common experience. A useful resource is healthtalk (formerly healthtalkonline) that proposes ‘reliable health information from patients, to patients’. It covers a large number of health conditions and for each topic around 40 video interviews have been recorded in which people share their experiences. The scientific information is accurate, exhaustive and non-judgmental.
The PATIENTS Program in the US is focused on research and the slogan ‘nothing about us without us’ sums this up looking for involvement of patients individually and collectively. In practice, it is difficult to know how to achieve patient and public involvement in research. The objective of this programme is to push people with experience of long-term illness to propose questions and actively participate in studies to answer them through innovative partnerships with patients involved at every step of the research process.
7. Conclusion
The results of EVE illustrate the difficulties encountered in the patient–healthcare provider relationship. Not all women who experienced symptoms that led to a significant worsening of their quality of life talked about it to their doctor and for those who did, the feeling of not being listened to was widely reported. In addition, nearly 20% of our respondents made the choice themselves to modify their treatment with the risk of decreasing the efficacy of their treatment. Websites facilitate access to health information giving wider access to resources but they could also reinforce inequalities if the person involved does not have the skills to use these resources efficiently. Next to health literacy improvement, it is of paramount importance to develop the empowerment of people living with chronic conditions so that they can have fruitful communication in healthcare settings. Finally, education programmes directed towards healthcare professionals are also an important contribution. Participatory research can help to document issues that are of concern in the complex patient–provider relationship so that relationships become a source of mutual and beneficial learning.
Author
Marguerite Guiguet is an epidemiologist at the French National Institute of Health and Medical Research (INSERM). She is currently working in clinical epidemiology of HIV infection with a focus on co-morbidities. Her partnership with the HIV/AIDS organisation AIDES was an opportunity to open her research interest to people’s needs.
References
Perdriger A. & Michinov E. (2015). ‘Therapeutic patient education: From infantilization to critical thinking’, Joint Bone Spine, 82, 299–301. Accessed 03/01/2016.
Wilson J. (1999). ‘Acknowledging the expertise of patients and their organisations’, BMJ, 319, 771–774.



